Abstract
Background: The beneficial effects of vitamin D, together with the high prevalence of vitamin D deficiency, have led to an expanding use of vitamin D analogues. While inappropriate consumption is a recognized cause of harm, the determination of doses at which vitamin D becomes toxic remains elusive.
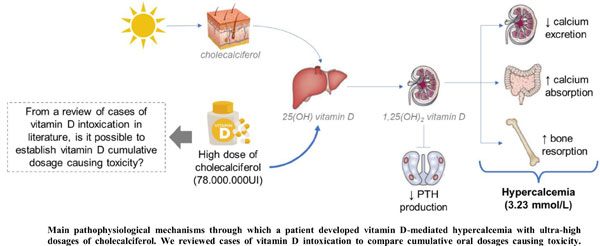
Case Presentation: A 56-year woman was admitted to our Hospital following a 3-week history of nausea, vomiting, and muscle weakness. The patient had been assuming a very high dose of cholecalciferol for 20 months (cumulative 78,000,000UI, mean daily 130,000UI), as indicated by a non-- conventional protocol for multiple sclerosis. Before starting vitamin D integration, serum calcium and phosphorus levels were normal, while 25OH-vitamin D levels were very low (12.25 nmol/L). On admission, hypercalcemia (3.23 mmol/L) and acute kidney injury (eGFR 20 mL/min) were detected, associated with high concentrations of 25OH-vitamin D (920 nmol/L), confirming the suspicion of vitamin D intoxication. Vitamin D integration was stopped, and in a week, hypercalcemia normalized. It took about 6 months for renal function and 18 months for vitamin D values to go back to normal.
Conclusion: This case confirms that vitamin D intoxication is possible, albeit with a high dose. The doses used in clinical practice are far lower than these and, therefore, intoxication rarely occurs even in those individuals whose baseline vitamin D serum levels have never been assessed. Repeated measurements of vitamin D are not necessary for patients under standard integrative therapy. However, patients and clinicians should be aware of the potential dangers of vitamin D overdose.
Keywords: Vitamin D, intoxication, overdose, cholecalciferol, toxicity, hypercalcemia.