Abstract
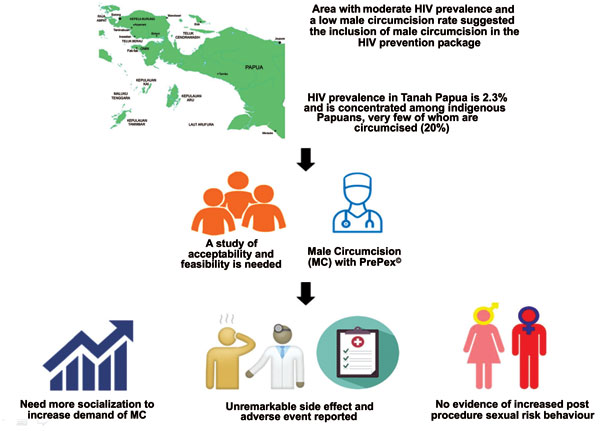
Background: Relatively little attention has been paid to the significant HIV prevention role that voluntary medical male circumcision (VMMC) can play in populations with moderate levels of HIV prevalence. One such location is Tanah Papua, Indonesia, which in 2013 had a general population having HIV prevalence of 2.3% concentrated among indigenous Papuans (2.9% prevalence), very few of whom are circumcised. This article reports the findings of an implementation research study assessing the acceptability and feasibility of introducing VMMC for HIV prevention.
Methods: Following a situational assessment and socialization of targeted groups of men and key stakeholders, a single-arm, open-label, prospective cohort trial using the non-surgical PrePex® device was undertaken in four cities. Study participants were recruited via study-associated socialization events. Data were collected from clients prior to and following device insertion, and at several “check-up” points (2-, 21- and 42-days) using standardized case report forms. A random sample of circumcision clients from one city was surveyed six months’ post-removal to assess the prevalence of compensatory sexual risk behaviours.
Results: Demand for circumcision was weak in three of the cities, reflecting insufficient prior socialization and lingering concerns over religious appropriateness and safety issues. Despite no prior experience with PrePex®, the pilot implementation yielded side-effect and adverse event rates that were unremarkable in comparison with sub-Saharan African countries, where PrePex® is widely used. No evidence of increased post-procedure sexual risk-taking was found.
Conclusion: The study findings point to both opportunity and significant challenges in introducing VMMC on a large scale in Tanah Papua, Indonesia. Although there were enough promising signs in the qualitative research and in the limited-scale implementation trial undertaken to remain optimistic as to the potential for VMMC to help contain HIV in Tanah Papua, much remains to be done to promote the benefits of VMMC and address lingering concerns as to safety and religious appropriateness. An acceleration of the pace of task-shifting from physicians to nurses will be needed in order for VMMC to be feasible for implementation on a large scale.
Keywords: Acceptability, feasibility, prepex®, tanah papua, Indonesia, voluntary male medical circumcision.